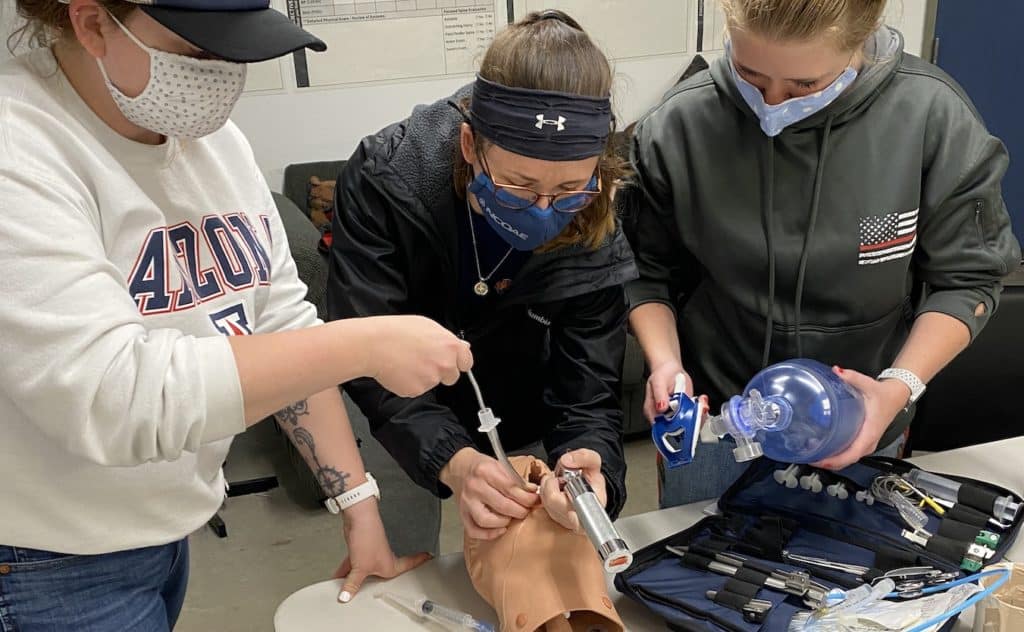
EMTs Come to the Rescue in Natural Disasters
Emergency MedicineThe morning of September 26, 2024, saw the peaceful mountain towns of western North Carolina waking up to their usual weather notifications. Even though the area was accustomed to storms, information about Hurricane Helene caused worry because it was growing stronger at a faster pace than anticipated.
The stronger the storm became, the greater the responsibilities of local Emergency Medical Technicians (EMTs). From organizing for the possibility of extensive evacuations to offering essential treatment in hazardous and uncertain settings, EMTs were at the ready.

Two recent hurricanes — Helene and Milton — serve as stark reminders that natural disasters can strike with little warning, leaving a trail of chaos and devastation in their wake. Saving lives and keeping people safe during a disaster, and cleaning up in its aftermath, requires the coordinated efforts of a diverse army of professionals, including doctors, police, members of the military, heavy-equipment operators, carpenters, electricians, plumbers, and more.
Also on the front lines are EMTs, such as the ones we train here at The National Center for Outdoor & Adventure Education, typically serving as part of the local rescue response. National emergency services, including the military and larger medical teams, are usually dispatched later. But they also require the dedication and expertise of EMTs.
In this post, I explore the indispensable contributions of EMTs during natural disasters, highlighting their training, the challenges they face, and the profound impact they have on (more…)
EMT Health and Fitness: How to Stay Physically Strong and Mentally Sharp
Emergency MedicineIt’s been my experience that emergency medical personnel — including Emergency Medical Technicians (EMTs) — tend to be much better at caring for others than for themselves. That’s generally the result of long shifts, life-or-death situations, and consistently helping people who are suffering the worst day of their lives. It’s going to take a toll.
To compound the problem, those who work in emergency medicine often neglect their own health and fitness. They forgo exercise, reach for junk food because it’s often handier. Or they begin to seek out various substances to get through the day. These might include energy drinks during their shift so they can remain alert. Or maybe a drink or three when they’re off the clock to calm their nerves and help them sleep.
Eventually, this unhealthy lifestyle catches up to them, negatively impacting their mood, energy, intimacy, and more.

The multi-billion dollar a year health and fitness industry offers little in the way of relief for those in our field. And often overlooked is the overworked and stressed-out Emergency Medical Systems (EMS) shift worker.
If you’re a member of that demographic or you’re considering an EMT training and certification program like our Standard EMT, Hybrid EMT, or Wilderness EMT, don’t wait around in the hopes of that industry or even your own EMS unit will be reaching out to you. Make this your wake-up call. Now is the time to start focusing on your own health and fitness.
Remember the lesson you’re taught when you board an airplane — put your oxygen mask on first before helping anyone seated next to you with theirs. In the same way, you need to focus on your own health first in order to be healthy and fit enough to assist others when they’re experiencing a medical emergency. And continue that health regimen so you are healthy enough to make a lasting career in emergency medicine.
In this post, I provide practical advice on how to restore and maintain your own physical and mental health and fitness over the long haul.
Manage Stress
Stress kills. We are all well aware of its negative impact on health, but what we need to realize is that a great deal of our stress is self-inflicted. After all, we’re the only ones who can (more…)
Spinal Immobilization or Spinal Motion Restriction: Which is Safest?
Emergency MedicineFor decades, spinal immobilization (SI) has been the standard practice when moving trauma patients with potential spinal injuries. Indeed, this particular procedure has long been commonplace for patients injured in the backcountry. Spinal immobilization involves the use of various devices, including a long spine board (LSB) and a cervical collar to stabilize the spine and prevent further injury.
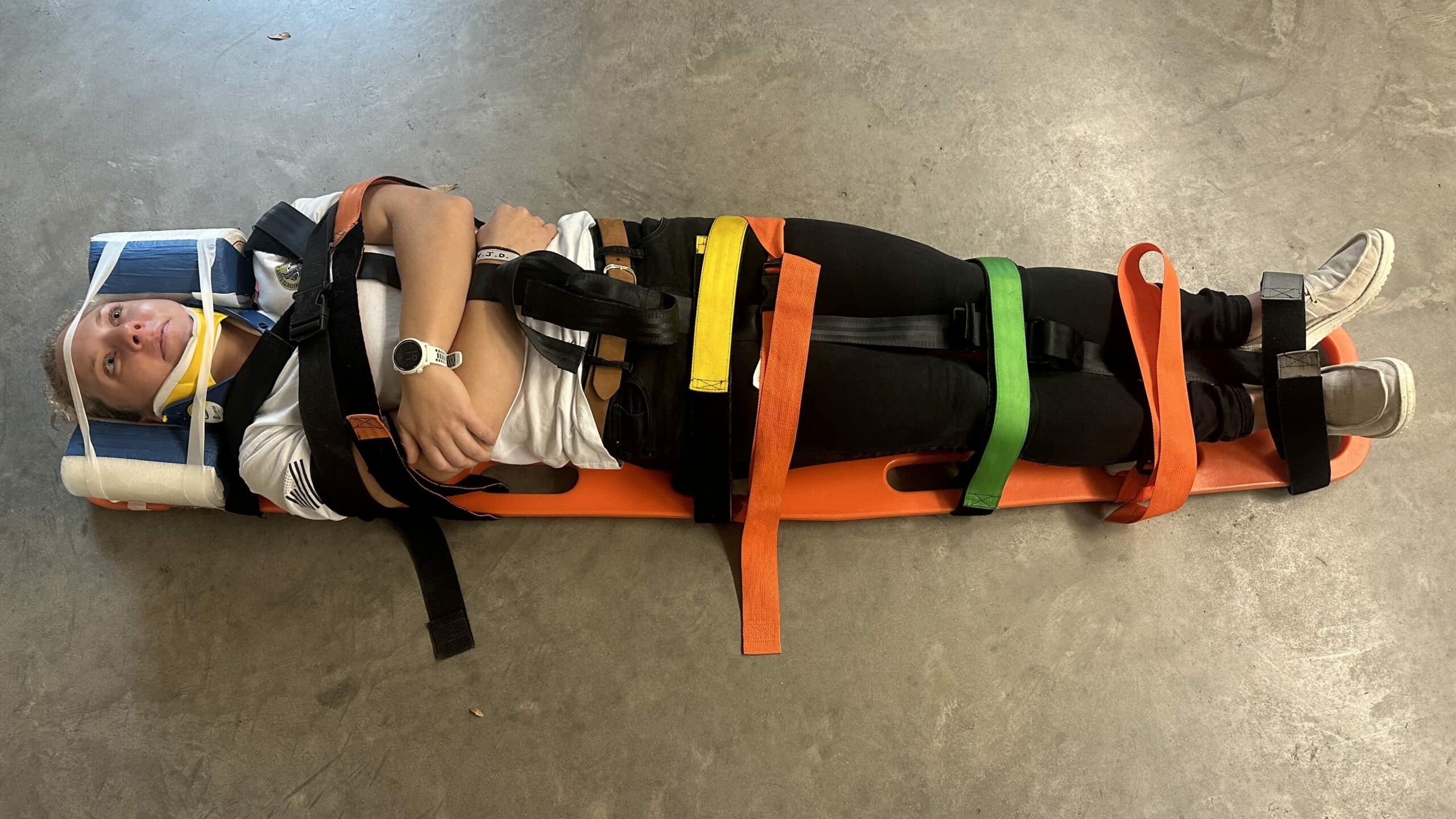
However, recent research has called this practice into question. In fact, while current techniques limit or reduce undesired motion of the spine, they do not succeed in fully immobilizing the spine. For this reason, the term “spinal motion restriction (SMR)” has gained favor over “spinal immobilization.”
Both terms refer to the same concept — minimizing unwanted movement of the potentially injured spine. However, while LSBs have historically been used to attempt spinal immobilization, SMR may be achieved using a scoop stretcher, vacuum splint, ambulance cot, or other similar device to which a patient is safely secured.
The National Registry of Emergency Medical Technicians (NREMT) defines the term “spinal immobilization” as the use of adjuncts (LSB, cervical collar, etc.) to prevent movement of the spine. The term “spinal motion restriction” is defined more broadly as attempting to maintain the spine in anatomic alignment and minimizing gross movement — irrespective of adjuncts.
Evaluating the Efficacy of Spinal Immobilization
The effectiveness of the LSB to prevent further trauma to the spine has never been proven in high-level trials. Its use was adopted largely by consensus and not driven by data from any formal studies. An extensive literature review on the history of not using the LSB as a tool concluded that it is ineffective and may be detrimental by delaying time-sensitive treatments for some patients.
A study published by Cambridge University Press examined patient outcomes over a decade during which Emergency Medical Service (EMS) systems decreased backboard use as they transitioned from SI to SMR protocols. The study included (more…)
Maintaining Resilience and Mental Health in the EMS Profession
Emergency MedicineThe suicide rate among emergency medical service (EMS) professionals rose a shocking 38 percent since 2009, according to a study published in the Western Journal of Emergency Medicine. But as shocking as that statistic is, it should come as no surprise.
As an emergency medical technician (EMT) or paramedic, you typically work a five-day rotation of 12-hour shifts (days or nights). You may start the week working Monday and Tuesday and then have Wednesday and Thursday off. You spend half your first day off catching up on sleep, doing chores, and running errands. You’re free the next day, but pretty much alone because everyone you know is at work or school or busy with other normal weekday obligations.

As a result, you likely lack the social connections many of us rely on for emotional support and psychological well-being. Come Friday, Saturday, and Sunday — when your friends and family are off work — you’re back on the job, providing critical medical care in highly stressful situations involving people who don’t always treat you with the respect and appreciation you deserve. And you have to perform this service with a smile on your face, because you don’t want a complaint on your record.
To make matters worse, emergency medical care leaves no room for mistakes. Quality assurance (QA) and quality improvement (QI) programs ensure that Monday morning quarterbacks are always looking over your shoulder to spot mistakes and offer their criticism and sage advice from their comfortable seats along the sidelines.
It’s Getting Worse Instead of Better
Thanks to high healthcare costs and doctor shortages, many people don’t have access to (more…)
Opinion: There’s Nothing “Basic” About an EMT
Emergency MedicineIt’s been more than a decade since the National Registry of Emergency Medical Technicians (NREMT) stopped using the certification designations EMT-B and EMT-Basic.
The change from EMT-B to EMT was not just in title. It was accompanied by an expanded set of knowledge and skill expectations for emergency medical technicians (EMTs). There is nothing “basic” about what an EMT learns or the skills he or she can perform. And they’re certainly not “Ambulance Drivers.”
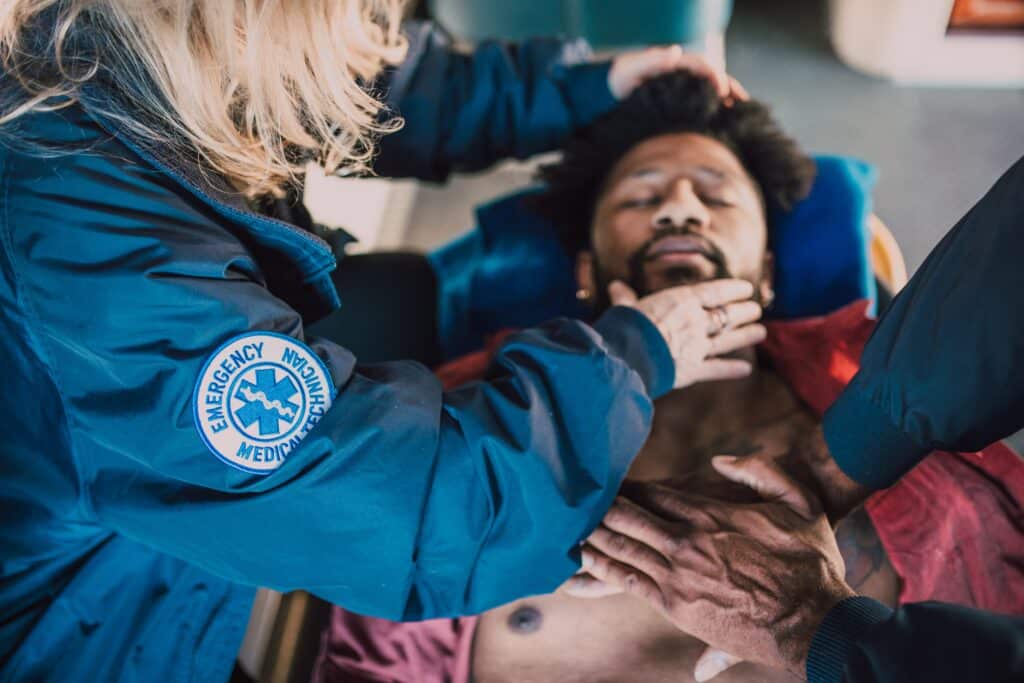
Most states have made the transition to the new title, but many emergency medical service (EMS) providers continue to refer to some EMTs as “Basics.” Maybe it’s out of ignorance, or just an antiquated habit, but we need that to stop. It’s much more than just an inaccurate designation — it’s misleading to the public and gives the wrong impression regarding care and capabilities.
Looking Back at EMT Designations
The early terminology came from a haphazard system of state-by-state naming conventions. The NREMT itself started out with an “EMT-Ambulance” or “EMT-A,” later adding an “EMT-Non-Ambulance” designation. As a result of this confusing (more…)
8 Alternative Jobs to Pursue with an EMT Certification
EMT TrainingJust obtaining an Emergency Medical Technician (EMT) license opens a world of career possibilities both inside and out of the medical field. Sure, you have to put in the effort, but the opportunities are as diverse as our EMT students here at The National Center for Outdoor & Adventure Education (NCOAE).
Fact is, we receive applications from students from all walks and stages of life, who successfully complete our EMT training program and go on to use that EMT training for a variety of opportunities. Some become full- or part-time EMTs, others use this outstanding training and education as a steppingstone for medical or nursing school. And then there are the outdoor enthusiasts who use this EMT training to become Ski Patrollers or members of Search and Rescue crews, or to add an additional layer of medical expertise when guiding groups on mountaineering and backcountry expeditions.

Maybe you’ve been an EMT for a while and are looking for a change, Or maybe you’re thinking about obtaining your EMT certification and then consider your options. While the most popular career trajectory for EMTs is to become a Paramedic, there are a number of jobs that you can obtain with just an EMT certification, keeping mind that some may require additional training.
Here are eight such opportunities: (more…)
Most EMS Terminology Comes Down to Initials, Abbreviations and Acronyms
EMT TrainingA few years ago, we ran a three-part series on slogans, slang, and terminology as it applies to a trio of human-powered outdoor recreational activities. If you recall, we started out with some “gnarly” surfing terms, then we “tied in” to a conversation about climbing, finally pulling a “wet exit” on the language of paddling.
You can review these three articles using the links below:
- From Sept. 20, 2020: Surfing Terminology and Slang: You Can’t Play BINGO Without the Lingo
- From Oct. 10, 2020: On Belay — Climbing Terminology and Slang
- From Oct. 30, 2020: Paddling Terminology and Slang: Nobody Says ‘Up a River Without an Oar’
There was quite a bit of word whimsy in those articles, and we made sure to remind readers that successfully lassoing the linguistics of a particular activity was no guarantee you were mastering that particular sport professionally.

Today we’re taking a more serious look at language, this time highlighting the terminology used by members of the Emergency Medical Service (EMS) community. That’s because one of our areas of focus here at The National Center for Outdoor & Adventure Education (NCOAE) is emergency medicine training and education. And whether you’re an EMS, medical professional, or wilderness first responder (WFR), these terms are most often employed when these professionals find themselves managing a medical emergency.
First off, you might notice that most of these terms come in the form of acronyms, abbreviations, and initials, and the reason for that is to enable first responders to quickly communicate and react with each other and the patient in the field.
The source for these acronyms comes from the NCOAE Wilderness Medicine Field Guide (ISBN 978-0-578-87449-4).
Here, we present them in alphabetical order: (more…)
NCOAE’s EMT Training Opens the Doors to Jobs Across the U.S.
EMT TrainingApplicants to our nationally renowned EMT training courses often ask us if they can take
their new EMT credentials to the state where they live, and the answer is mostly yes.
The National Center for Outdoor and Adventure Education’s (NCOAE) campus is
located in North Carolina, where we offer 21-day “Intensive” EMT-Basic and 23-day
“Intensive” Advanced EMT training courses among others. Successful completion of
these courses authorize our graduates to take the National Registry of Emergency
Medical Technicians (NREMT) exam.

National Registry Certification examinations evaluate the competence of EMS
practitioners at a variety of levels, including Emergency Medical Responder (EMR),
Emergency Medical Technician (EMT), Advanced Emergency Medical Technician
(AEMT), and Paramedic.
NREMT credentials are either required for an initial license or accepted for legal
recognition or reciprocity in all 50 states and Puerto Rico. That makes it easier to
maintain
Exactly What Is It That an EMT Does?
EMT TrainingDepending on where you live, you may see them every day or just when there’s a fire, police, or medical emergency where you are. Regardless of the frequency with which you see them, you may be wondering — what exactly does an EMT (Emergency Medical Technician) do?
EMTs are not just “ambulance drivers,” although that’s certainly a critical part of their occupation. An Emergency Medical Technician is a trained and certified medical provider who has demonstrated competency in basic pre-hospital medical care.
For EMTs and patients, an ambulance is more than transportation to the hospital. It’s a mobile mini-medical center squeezed into the back of a moving vehicle where a skilled team of pre-hospital healthcare providers perform a variety of life-saving medical interventions that save lives every day in every community.
What an EMT Must Learn
While nearly anyone can attempt to become an EMT, in order to qualify to take and pass the National Registry of Emergency Medical Technicians certification exam, candidates must first complete an approved EMS education program. In that program, EMT candidates’ study and learn a lot of things, including:
(more…)How to Become an EMT
EMT TrainingYou’re thinking about becoming an EMT. Awesome! If you follow through, you will be joining the ranks of today’s modern-day heroes, the frontline of the frontline workers — bona fide life savers!
Emergency Medical Technicians (EMTs) are trained professionals who provide care in critical and emergency situations. Such emergencies can range from simple, routine calls to intense and complex scenarios.
You may show up for a call only to discover that there is no victim, or the person is okay and refuses help, or a patient simply needs transportation from one medical facility to another. On the other hand, you could be called in to attend to the victim of a car accident or a shooting or a heart attack, drowning, mountaineering accident, or drug overdose. You may even have to deliver a baby! You can never predict what will happen over the course of any given shift.
As an EMT, your job responsibilities generally boil down to keeping patients alive using non-invasive medical procedures and transporting them safely to a hospital or clinic where they can receive a higher level of professional medical care. More specifically, you have three fundamental job responsibilities:
- Assessment and stabilization of the patient’s condition
- Basic life support
- Transportation
In this post, we bring you up to speed on the different levels in emergency medicine and credentialing while explaining the basic education and skills required to become an EMT.
(more…)Meet the Student: Gordon Harrison III
Student ProfilesIf Gordon Harrison’s name sounds familiar to you, that likely means one of two things: You either know him personally or you’re a fan of the water sport known as wakeboarding.
David “Gordon” Harrison (the third) recently graduated from one of our 19-Day ‘Intensive’ EMT-Basic training courses. And as you probably figured out by now, this native of Caroline County, Va. (who now calls Melbourne Beach, Fla. his home), holds the distinction of being the only professional athlete to enroll in that course — or any course for that matter here at The National Center for Outdoor & Adventure Education.
Harrison started wakeboarding as a child and become good enough in high school to be invited by the World Wake Association to join the Jr. Pro Wakeboard Tour. Suffice to say, he’s never looked backward since.
For the uninitiated, wakeboarding is a water-based sport in which the athlete — standing on a short board with foot bindings known as a wakeboard— is towed behind a motorboat across its wake, allowing the athlete to crest the wake for aerial maneuvers. In Harrison’s case, he’s so proficient at wakeboarding that he’s only one of a handful of people on the planet capable of making a living as a professional wakeboarder.
So, what possesses someone living the life of a pro athlete to drop everything and spend 19 days with us in North Carolina preparing to sit to for the NREMT (National Registry of Emergency Medical Technicians) exam? That’s what we wanted to know. Here’s what Harrison had to say, in his own words: (more…)
TALK TO US
Have any further questions about our courses, what you’ll learn, or what else to expect? Contact us, we’re here to help!