Spinal Immobilization or Spinal Motion Restriction: Which is Safest?
December 11, 2023
For decades, spinal immobilization (SI) has been the standard practice when moving trauma patients with potential spinal injuries. Indeed, this particular procedure has long been commonplace for patients injured in the backcountry. Spinal immobilization involves the use of various devices, including a long spine board (LSB) and a cervical collar to stabilize the spine and prevent further injury.
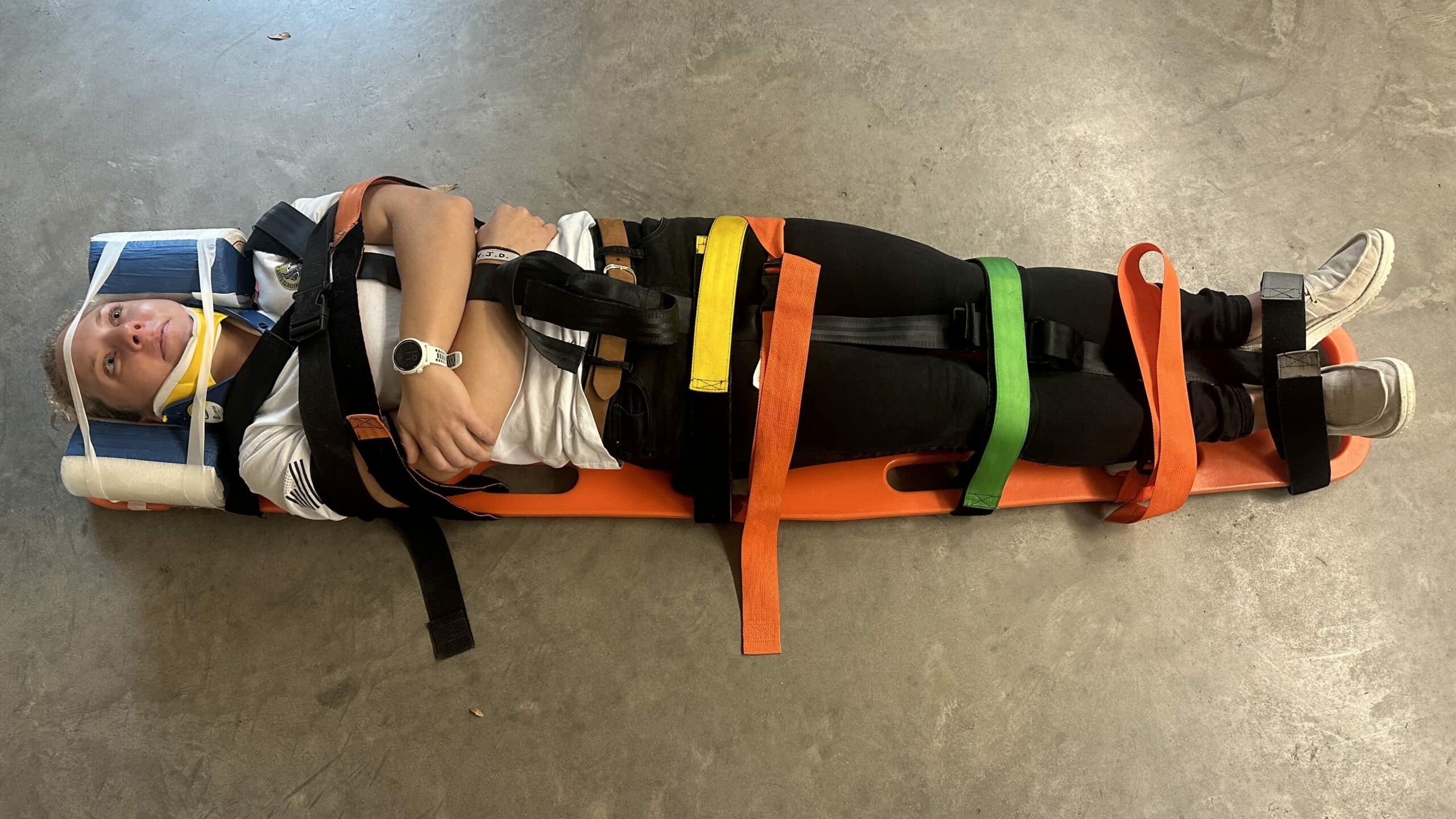
However, recent research has called this practice into question. In fact, while current techniques limit or reduce undesired motion of the spine, they do not succeed in fully immobilizing the spine. For this reason, the term “spinal motion restriction (SMR)” has gained favor over “spinal immobilization.”
Both terms refer to the same concept — minimizing unwanted movement of the potentially injured spine. However, while LSBs have historically been used to attempt spinal immobilization, SMR may be achieved using a scoop stretcher, vacuum splint, ambulance cot, or other similar device to which a patient is safely secured.
The National Registry of Emergency Medical Technicians (NREMT) defines the term “spinal immobilization” as the use of adjuncts (LSB, cervical collar, etc.) to prevent movement of the spine. The term “spinal motion restriction” is defined more broadly as attempting to maintain the spine in anatomic alignment and minimizing gross movement — irrespective of adjuncts.
Evaluating the Efficacy of Spinal Immobilization
The effectiveness of the LSB to prevent further trauma to the spine has never been proven in high-level trials. Its use was adopted largely by consensus and not driven by data from any formal studies. An extensive literature review on the history of not using the LSB as a tool concluded that it is ineffective and may be detrimental by delaying time-sensitive treatments for some patients.
A study published by Cambridge University Press examined patient outcomes over a decade during which Emergency Medical Service (EMS) systems decreased backboard use as they transitioned from SI to SMR protocols. The study included 549 patients in the SI period and 623 patients in the SMR period. Authors of the study concluded that the change from an SI to an SMR protocol “did not demonstrate a significant effect on the incidence of disabling spinal injuries.”
The Eastern Association for the Surgery of Trauma (EAST), the National Association of EMS Physicians (NAEMSP), and the American College of Surgeons Committee on Trauma (ACS-COT) all support the recommendation against the use of spinal immobilization in patients with isolated penetrating injuries. They all point to the research that shows that spinal immobilization is associated with increased mortality and neurologic injury. Furthermore, studies demonstrate that SI has no benefit in preventing neurological deficits, even potentially reversible neurologic deficits.
Evaluating the Efficacy of Spinal Motion Restriction
The amount of acceptable motion in a patient with a spinal cord injury is unknown. A small amount of motion is unlikely to result in additional damage to the spinal cord, and any subsequent injury could be related to ischemia (restricted blood flow to the damaged area) and swelling.
A common concern is that SMR is inadequate to prevent movement in patients with spinal injuries and will lead to harm. Whether this is true is unclear at this time and will be difficult to ascertain because of the infrequency of spinal injuries. According to the National Association of EMS Physicians (NAEMSP), more than 13 million people in the United States seek care in emergency departments for cervical spine injuries, but only 0.3 percent have actually sustained a significant neurologic injury.
The cost of radiographic tests for these patients is estimated at more than $180 million. Among trauma patients, only 1 percent involve cervical spine injuries and only 0.3 percent involve injury to the spinal cord. Such low incidences of significant injury indicate that a very large patient population would be necessary to identify injuries missed by SMR.
Limiting the Use of the Long Spine Board
The NAEMSP and the American College of Emergency Physicians (ACEP) have both recommended limiting the use of the long spine board (LSB) and moving from spinal immobilization to spinal motion restriction with a rigid cervical collar. The NAEMSP position paper and supporting resource document states that a patient with neurologic deficit and spinal pain or tenderness may be placed on an LSB, but the LSB should be considered an extrication device only, with the patient being removed from the LSB as soon as possible.
The NAEMSP does not differentiate athletes from the general population. If you are an athletic trainer, recognize that local EMS agencies may use long spine boards routinely (and typically rarely) to manage athletes with suspected spine injuries, along with alternative methods, as outlined in the venue emergency action plan and the pregame medical time-out. Unique settings and situations such as the gymnastics pit, swimming pool, and equipment-laden athletes deserve special attention in the emergency action plan.
My Experience with Spinal Motion Restriction
My EMS experience supports the data. When responding to patients with potential or suspected spinal injuries, I have found that the use of a long spine board and full spinal immobilization was detrimental to patient comfort, outcome, and safety. In nearly all of my transports to the emergency department of a patient on a long spine board, it was removed almost immediately by the physician.
I believe we do less harm to the patient, optimize patient care, and provide faster transport to the emergency department (when necessary), without spinal immobilization. But that requires proper mainline stabilization and C-spine protocols with the option for spinal motion restriction.
= = = = = = = =
About the Author: David Bullard is the Director of Emergency Medicine Education at The National Center for Outdoor & Adventure Education (NCOAE) in Wilmington, North Carolina.
TALK TO US
Have any further questions about our courses, what you’ll learn, or what else to expect? Contact us, we’re here to help!
Leave a comment